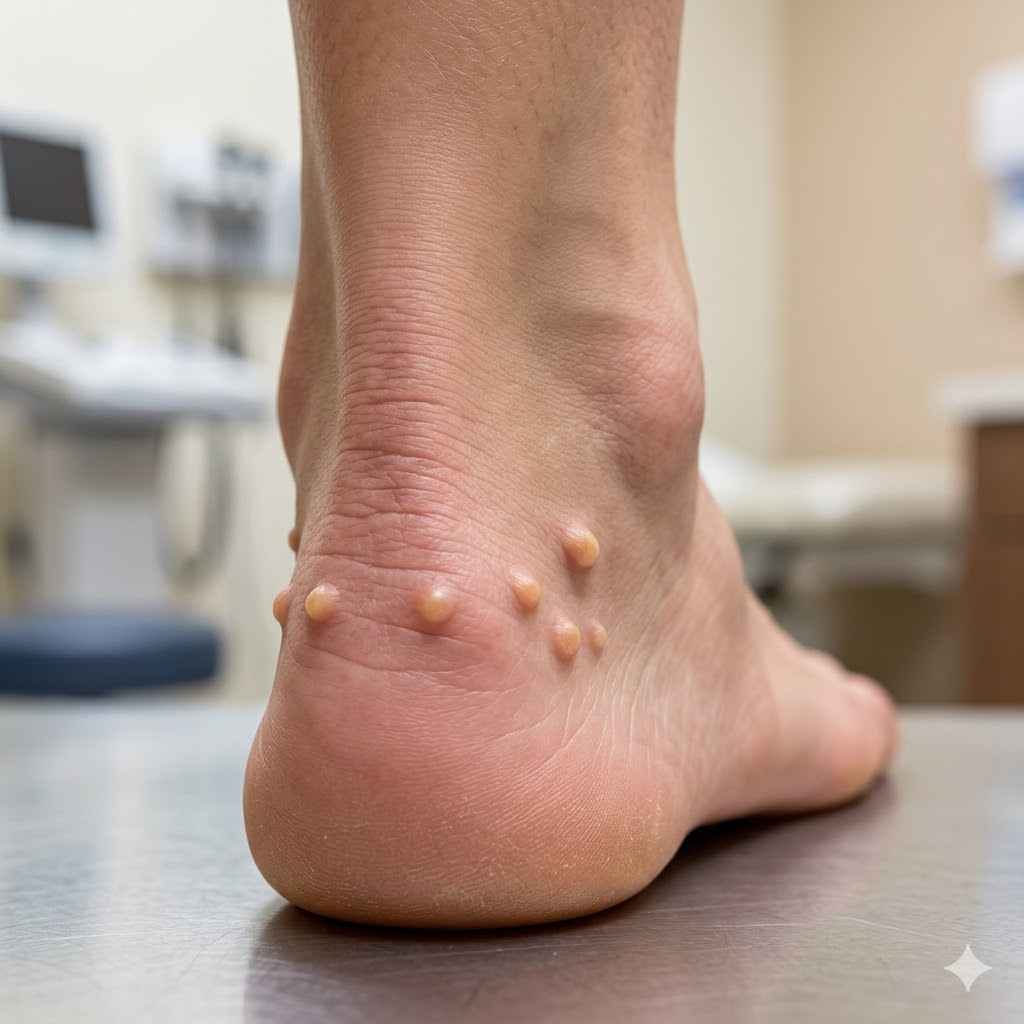
Piezogenic pedal papules are small, skin-colored bumps that appear on the feet. They become more visible when standing or putting weight on the feet. They are generally harmless and do not require treatment. The exact number of people with them is not precisely known, but they are considered quite common, especially in adults.
What Are Piezogenic Pedal Papules?
Piezogenic pedal papules (PPPs) are small, soft bumps. They show up on the feet. This usually happens on the sides.
The word “piezogenic” means pressure-causing. So, these bumps come out with pressure. This pressure often comes from standing or walking.
They are most noticeable when you are on your feet.
When you stand, your feet take on more weight. This pressure makes the bumps appear. When you lift your foot, they often go away.
This is a key sign. The bumps are usually the same color as your skin. They can sometimes look a bit darker.
They are not painful for most people.
These papules are made of fat. Specifically, they are small herniations of fat. This fat pushes through weak spots in the connective tissue.
This tissue surrounds your skin and muscles. Think of it like a small bulge. It happens where the tissue is a bit thinner or less strong.
The exact medical term can sound big. But the idea is simple. It’s a bit of fat pushing out where it’s a little weaker.
This happens on your feet. It’s very common. Many people have them and don’t even know it.
Or they notice them but don’t think much of it.
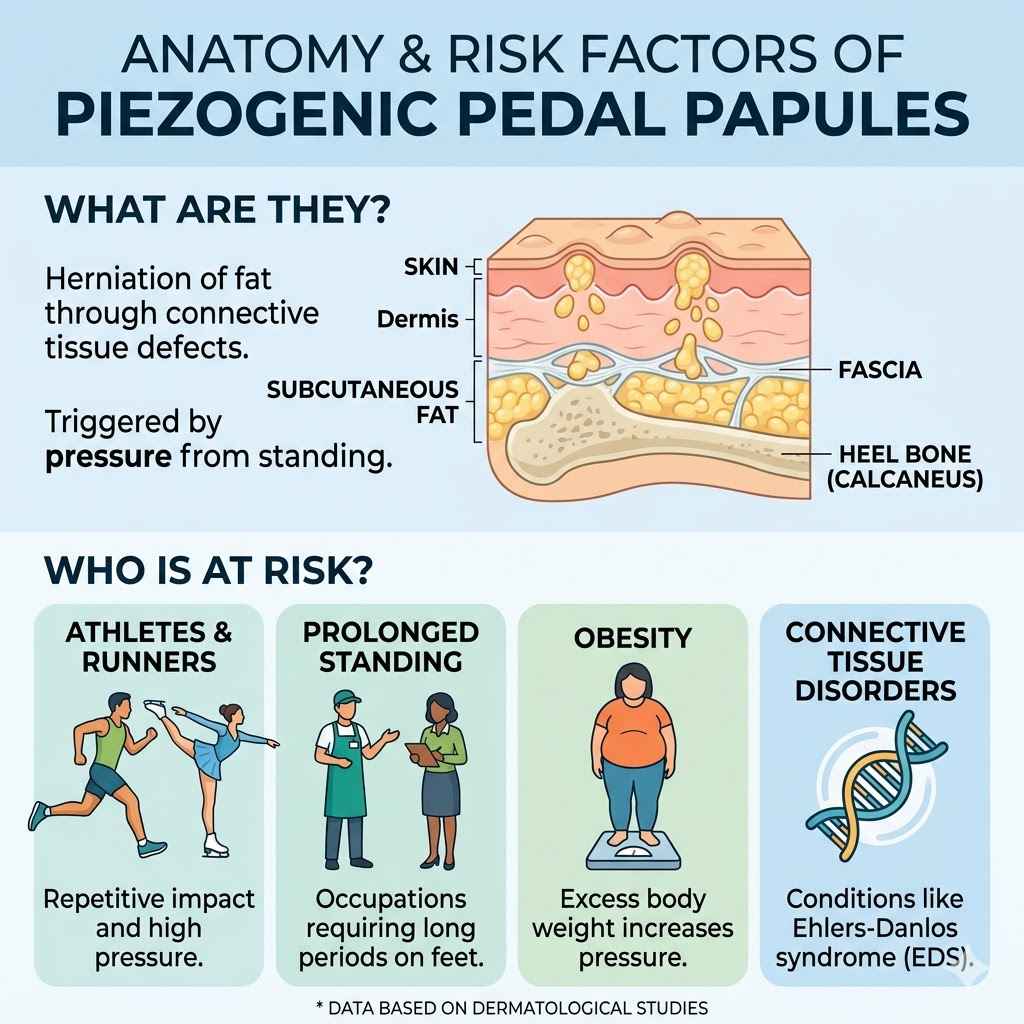
Why Do Piezogenic Pedal Papules Happen?
The main reason for piezogenic pedal papules is pressure. When you stand, your weight presses down on your feet. This pressure can force small pockets of fat to push through the skin.
It’s like squeezing a tube of toothpaste. The paste comes out where it can.
There are a few things that make them more likely. One is standing for a long time. If your job keeps you on your feet all day, you might notice them more.
Athletes, especially runners or those who stand a lot, can also get them. Their feet are under constant stress.
Age plays a role too. As we get older, our skin and connective tissues can lose some of their firmness. This can make them more prone to these small fat bulges.
So, they tend to show up more in adults than in children. They are rarely seen in very young kids.
There’s also a link to certain medical conditions. Some studies suggest a connection to conditions that affect connective tissue. Things like Ehlers-Danlos syndrome are sometimes mentioned.
This is where your connective tissues are more stretchy than usual. However, most people who get PPPs have no other health issues.
So, it’s a mix of factors. It’s often just normal body changes. The way your feet are built matters.
The amount of time you spend standing matters. And how your skin and fat are structured matters. For most, it’s not a sign of something bad.
It’s just how some feet react to pressure.
Common Triggers for Piezogenic Pedal Papules
Standing for long periods: This is the biggest factor. Jobs requiring lots of standing can make them appear.
Physical activity: Running, jumping, and sports that stress the feet can be a trigger.
Aging: Skin and connective tissue lose some elasticity over time.
Genetics: There may be a hereditary component for some people.
Obesity: Extra weight can increase pressure on the feet.
How Common Are They Really?
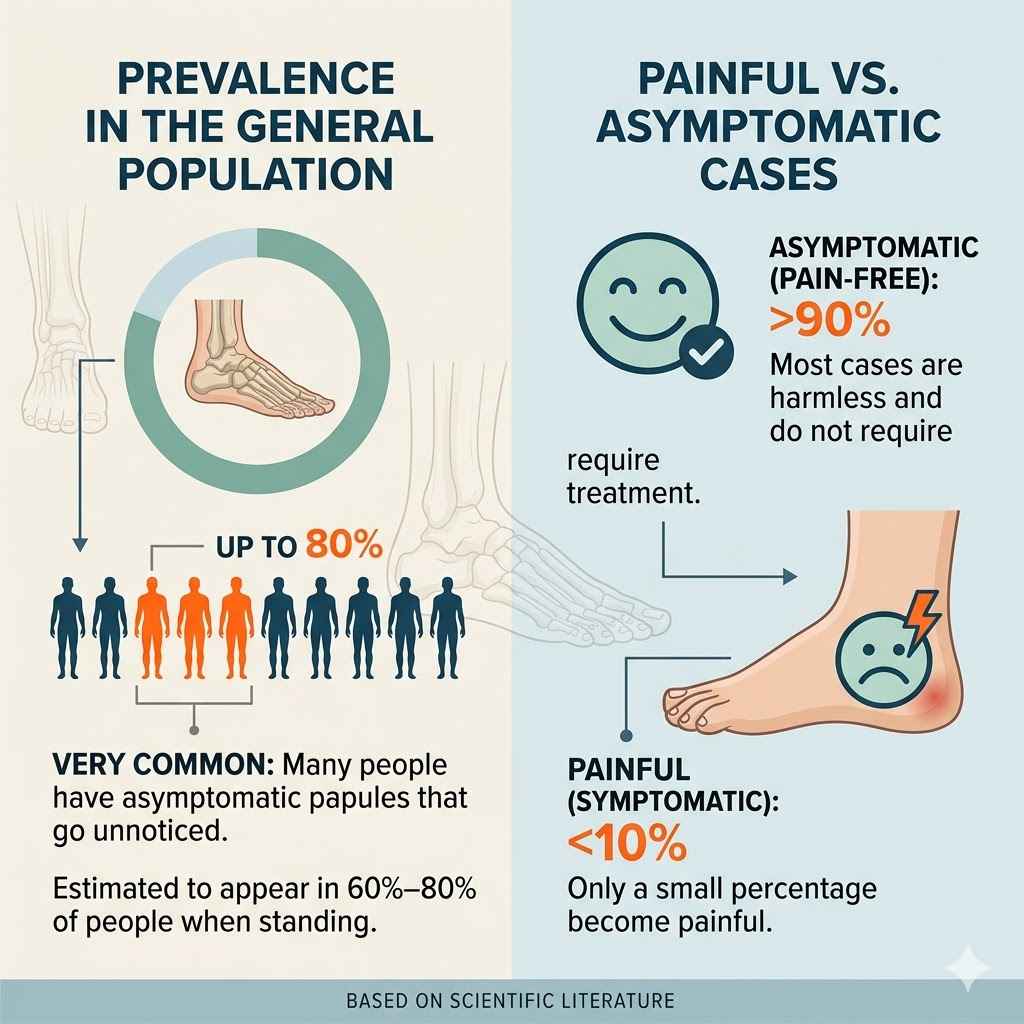
It’s tough to give an exact number for how many people have piezogenic pedal papules. There isn’t a big study that counted every single person. But doctors and researchers agree they are very common.
Some estimates suggest a large portion of the adult population may have them.
Think about it this way: most people don’t go to the doctor for them. They see them, wonder about them, and then often forget about them. They don’t cause pain.
They don’t usually look bad enough to seek medical help. So, many cases likely go unreported.
One study looked at college students. It found that about 20% of them had PPPs. Another study, looking at people in a clinic, found them in about 40% of patients.
These are just snapshots. But they show that it’s not rare. It’s quite frequent.
Consider the factors we talked about. Standing is common. Aging is universal.
Most adults have experienced these. So, it makes sense that the numbers are high. It’s possible that up to half of all adults might have them.
Some might have just one or two. Others might have several.
What’s important to understand is that having them is usually normal. It doesn’t mean you have a serious illness. It’s a common physical trait.
Like having freckles or a certain hair type. It’s just part of how some people’s feet work under pressure.
Piezogenic Pedal Papules: Key Facts
Prevalence: Very common, likely affecting a significant portion of adults.
Age Group: More common in adults than children. Tend to appear with age.
Symptoms: Usually asymptomatic (no pain or itching). Visible with pressure.
Appearance: Small, skin-colored or slightly darker bumps on the sides of the feet.
Cause: Fat herniation through weak spots in connective tissue due to pressure.
My Own Experience with Foot Bumps
I remember one summer. I took up hiking more seriously. I was spending hours on my feet each weekend.
One day, after a particularly long trek, I was sitting down. I looked at my feet. I noticed these little bumps on the sides.
They were quite clear. I had never seen them before.
My first thought was panic. What were these things? Were they warts?
Something worse? I remembered reading health articles. I felt a slight unease.
It was that feeling of the unknown. I pressed on them. They seemed to flatten.
Then, when I stood up again, they popped back out.
I spent a few days looking them up online. I saw pictures that looked like mine. I read about piezogenic pedal papules.
The explanation made sense. My feet were under a lot of new stress. I was older than I used to be.
My skin probably wasn’t as tight. It was a relief to learn they were common and usually harmless.
I still get them after long hikes. They are a reminder of the pressure my feet are under. But now, I don’t worry.
I know what they are. It’s a strange feeling to have something on your body that you don’t want to go away. But for PPPs, that’s the case.
They are just part of life for many of us.
Personal Story: Noticing the Papules
The Moment: Noticed after a long period of standing.
Initial Reaction: Worry and confusion about their appearance.
Investigation: Researched online and found information on PPPs.
Understanding: Learned they are common fat bulges due to pressure.
Current View: No longer a cause for concern; accepted as a normal occurrence.
When Are Piezogenic Pedal Papules a Concern?
For most people, piezogenic pedal papules are not a problem. They are a common finding. They don’t usually cause pain or discomfort.
They don’t interfere with walking or daily activities. So, in most cases, you don’t need to do anything about them.
However, there are times when you should pay attention. If the bumps start to hurt, that’s a sign to see a doctor. Pain could mean they are getting irritated.
Or perhaps something else is going on. If they swell up or become red, that also warrants a look.
Sometimes, the bumps can become more prominent. They might look larger or more numerous. If this change happens quickly, it’s worth getting it checked.
While usually benign, rapid changes in any skin feature are good to discuss with a healthcare provider.
Also, if you have other symptoms along with the papules, see a doctor. For example, if you have joint pain, unusual fatigue, or skin changes elsewhere. This could point to an underlying condition.
As mentioned, PPPs can sometimes be associated with connective tissue disorders.
The key is to know your own body. If something feels off, it’s always best to get it checked. A doctor can look at the bumps.
They can confirm if they are indeed piezogenic pedal papules. They can also rule out other, less common, issues. It’s better to be safe than sorry.
Remember, the vast majority of PPPs are harmless. They are a cosmetic concern at most for some people. But they don’t signal a serious health threat.
Think of them as a little quirk of your feet. They are a sign your feet are working hard under pressure.
Signs That Might Warrant a Doctor’s Visit
Pain: Any discomfort or tenderness associated with the bumps.
Swelling: If the papules become noticeably swollen.
Redness: Inflammation or irritation around the bumps.
Rapid Change: If the size or number of papules increases very quickly.
Associated Symptoms: Other health issues occurring at the same time.
What Can You Do About Piezogenic Pedal Papules?
The good news is that for most people, you don’t need to do anything. Piezogenic pedal papules are typically harmless. They don’t require treatment.
Doctors usually advise leaving them alone. Trying to remove them often isn’t necessary and can sometimes cause other problems.
However, if they bother you cosmetically, there are some things you can try. The most straightforward approach is to reduce the pressure on your feet. This might mean taking breaks when standing for long periods.
Try to sit down and elevate your feet when you can.
Wearing comfortable shoes is also important. Shoes that offer good support can help. Avoid shoes that are too tight or put extra pressure on the sides of your feet.
This might make the papules less noticeable.
Some people try to avoid standing for long durations. If your job requires it, try to get short breaks. Even a few minutes can help reduce the sustained pressure.
This might not make the papules disappear completely. But it can lessen their prominence.
In rare cases, if the papules are very large or cause significant cosmetic concern, a doctor might discuss options. These are not common. They might involve procedures to reduce the fat.
But this is usually a last resort. And it’s not something done for typical PPPs.
The main takeaway is that treatment is rarely needed. Focus on comfort and reducing unnecessary pressure. If you’re worried, a quick chat with your doctor is always a good idea.
They can confirm the diagnosis and reassure you.
Tips for Managing Piezogenic Pedal Papules
Reduce Standing Time: Take breaks whenever possible.
Supportive Footwear: Wear shoes that fit well and offer good cushioning.
Elevate Feet: When resting, prop your feet up to relieve pressure.
Listen to Your Body: If they become painful or change, see a doctor.
Cosmetic Concern: If they bother you, focus on reducing pressure, not medical treatment.
Distinguishing PPPs from Other Foot Bumps
It’s good to know what you’re looking at. Feet can get all sorts of bumps and lumps. So, how do you know if what you have is a piezogenic pedal papule?
There are a few key ways to tell them apart from other common foot issues.
First, the timing. PPPs appear with pressure. This is their main characteristic.
When you stand or walk, they pop out. When you lift your feet or lie down, they often disappear. Most other bumps don’t behave this way.
Second, the location. PPPs typically form on the sides of the feet, especially near the heel or arch. You might see them on both feet.
They are not usually found on the soles of your feet or on your toes.
Third, the appearance. They are usually small, skin-colored bumps. They are soft to the touch.
They don’t typically have a rough or scaly surface like warts. They also don’t usually have a central pore or dimple like a blackhead. And they aren’t typically red and inflamed like an infection.
Warts (Plantar Warts): These are caused by a virus. They can be painful. They often have tiny black dots inside them.
They are usually rough on the surface. They don’t disappear when you take pressure off your foot.
Cysts: These are fluid-filled sacs. They can occur on the feet. They might be softer or firmer than PPPs.
They don’t necessarily appear or disappear with pressure. Some cysts can become inflamed and painful.
Corns and Calluses: These are thickened areas of skin. They form due to friction or pressure. They are usually flat or slightly raised.
They don’t pop in and out. They are a response to rubbing, not fat herniation.
Lipomas: These are benign tumors made of fat. They can occur anywhere on the body. They are usually softer and can be larger than PPPs.
They don’t necessarily change with pressure.
If you are unsure about a bump on your foot, it’s always best to consult a healthcare professional. They have the expertise to accurately diagnose what it is. They can tell you if it’s a common piezogenic pedal papule or something else that needs attention.
PPPs vs. Other Foot Bumps: A Quick Guide
Piezogenic Pedal Papules: Appear with pressure, disappear with rest. Skin-colored. Sides of feet.
Plantar Warts: Rough surface, tiny black dots. Can be painful. Don’t change with pressure.
Cysts: Fluid-filled sacs. May not change with pressure. Varying firmness.
Corns/Calluses: Thickened skin from friction. Flat or raised. Don’t pop out.
Lipomas: Soft fat tumors. Can be larger. Don’t change with pressure.
The Science Behind the Fat Herniation
To really understand piezogenic pedal papules, let’s dive a little into the science. The skin is held in place by a layer called the dermis. This dermis is made of connective tissue.
It’s like a supportive mesh. Underneath the dermis is subcutaneous fat. This is the layer of fat that cushions our bodies.
In certain areas, the connective tissue in the dermis can be a bit weaker. Or it might have natural openings. When you apply pressure to the foot, like when standing, this pressure is significant.
It pushes down on the fat layer. This pressure can force small amounts of fat to squeeze through these weaker spots or openings in the dermis.
This is called a fat herniation. The fat pocket bulges out. It pushes up against the skin.
This creates the visible bump. The skin itself isn’t weak. It’s the underlying connective tissue that has the slight weakness.
Think of it like a tiny hole in a strong fabric bag. If you push soft contents from inside, they’ll bulge through the hole.
Why do these weak spots happen? It’s often a combination of genetics and aging. Our bodies are all a little different.
Some people are born with naturally thinner or less dense connective tissue in certain areas. Over time, this tissue can also lose some of its strength and elasticity. This makes it easier for fat to push through.
Repetitive stress from walking and standing can also play a part. It’s constant pressure on the feet. This repeated force might make small weaknesses more apparent over time.
It’s not like a sudden injury. It’s more like wear and tear.
Understanding this science helps explain why PPPs are more common as people age. It also explains why they appear with pressure. The fat is always there.
The connective tissue is always there. But the interaction of pressure and the tissue’s structure makes the papules appear when they do.
Understanding Fat Herniation in PPPs
Connective Tissue: Forms a supportive mesh under the skin.
Subcutaneous Fat: The layer of fat below the dermis.
Weak Spots: Natural or age-related thinning in the connective tissue.
Pressure: Standing and walking force fat through these weak spots.
Herniation: A small bulge of fat pushing against the skin.
Impact on Foot Health and Well-being
For the vast majority of people, piezogenic pedal papules have zero impact on their foot health or overall well-being. They are a benign finding. They don’t cause any medical problems.
You can walk, run, and live your life normally with them.
The only way they might impact well-being is if they cause worry or self-consciousness. If someone is very aware of them, they might feel anxious. This is understandable.
But it’s important to remember they are incredibly common. Many, many people have them.
If they were to become painful or inflamed, then they would impact well-being. But this is rare. In such cases, it’s not the PPP itself causing the problem, but an associated issue like irritation or infection.
Then, it would be treated like any other painful foot lesion.
Some people might wonder if they affect athletic performance. Unless they are causing pain or discomfort, they do not. The physical presence of these small fat bulges does not hinder the mechanics of your foot.
Your ability to move is not compromised.
It’s good to have them checked by a doctor if you are concerned. This professional evaluation is key. It can confirm they are indeed PPPs.
This confirmation can relieve a lot of anxiety. Knowing it’s a normal, harmless thing is powerful.
So, in summary, the impact is minimal to none for most. They are a cosmetic or observational finding. They don’t require medical intervention and don’t usually affect your quality of life.
Their main “impact” is often the questions they raise in our minds!
Impact of Piezogenic Pedal Papules
Health Impact: Generally none. They are benign.
Pain/Discomfort: Rare. Usually not associated with PPPs themselves.
Activity Level: Do not affect walking, running, or sports.
Psychological Impact: Can cause worry or self-consciousness if unknown.
Medical Intervention: Rarely needed, as they are not a disease.
When is it Time to See a Doctor?
As we’ve touched upon, seeing a doctor for piezogenic pedal papules isn’t usually necessary. But there are specific times when it’s a good idea to seek professional advice. These situations help ensure your foot health and peace of mind.
1. Persistent Pain: If the bumps are consistently painful, especially when you walk or wear shoes, it’s time for a visit. Pain isn’t a typical symptom of PPPs.
It might signal irritation or a different issue.
2. Rapid Changes: If you notice the papules suddenly becoming much larger, more numerous, or changing in texture, see a doctor. Quick changes can sometimes indicate something more needs investigation.
3. Redness or Swelling: Signs of inflammation like redness, increased warmth, or swelling around the bumps are reasons to consult a healthcare provider. This could mean an infection or irritation.
4. Uncertainty: If you are simply unsure what the bumps are. A doctor can examine them.
They can provide a diagnosis and explain what they are seeing. This is often the quickest way to get reassurance.
5. Associated Symptoms: If you have other health concerns along with the foot bumps. This includes joint pain, skin rashes elsewhere, or unusual fatigue.
These might point to a systemic condition.
6. Cosmetic Concern (and you want options): While not a medical necessity, if the papules are a significant cosmetic concern for you and you wish to discuss potential (though rare) management options, your doctor can guide you.
When you see a doctor, they will likely ask about when you noticed the bumps. They’ll ask about pain or other symptoms. They will then examine your feet.
Often, they can diagnose PPPs just by looking. They might ask you to stand up. This helps them see the papules appear.
Don’t hesitate to make an appointment if you have any doubts. Your foot health is important. A doctor’s visit can provide clarity and peace of mind.
When to Consult a Doctor About Foot Bumps
Pain: If the bumps are painful.
Changes: If they grow quickly or change texture.
Inflammation: If they are red or swollen.
Doubt: If you are unsure of the diagnosis.
Other Issues: If accompanied by other health symptoms.
The Role of Genetics and Family History
Like many things about our bodies, genetics can play a role in piezogenic pedal papules. While pressure is the direct trigger, how our bodies respond to that pressure can be influenced by our genes. Some people may inherit a predisposition to having weaker connective tissue in their feet.
This means that for some families, PPPs might be more common. If your parents or close relatives have them, you might be more likely to develop them too. This doesn’t mean everyone in that family will have them.
But the tendency might be there.
It’s not typically a single gene that causes them. It’s more likely a complex interplay of several genes. These genes influence the strength, elasticity, and structure of connective tissues.
They also influence how skin and fat layers are organized.
If you have a family history, it doesn’t mean you’re guaranteed to get them. Many other factors are involved, like lifestyle and age. However, knowing your family history can be helpful.
It can prepare you for the possibility. It might also make you more likely to recognize them if they appear.
Doctors sometimes ask about family history when diagnosing conditions. For PPPs, it’s part of the overall picture. It helps them understand the potential contributing factors for an individual.
It’s another piece of the puzzle. But it’s rarely the only piece.
So, while genetics can predispose you, it’s the everyday pressure on your feet that brings them to light. It’s a great example of how our genes and our environment work together. They shape our bodies and the way they function.
Genetic Factors in Piezogenic Pedal Papules
Predisposition: Genes can influence connective tissue strength.
Family History: May be more common in some families.
Complex Inheritance: Likely influenced by multiple genes.
Interaction: Genes work with lifestyle and age.
Awareness: Family history can increase recognition.
Understanding the Numbers: Why Exact Counts Are Difficult
As an AI, I can’t offer personal experience, but I can tell you that getting precise numbers for conditions like piezogenic pedal papules is often tricky. It’s not like counting people with a specific allergy or a measurable condition like diabetes.
Why is it hard to get an exact count? Several reasons come to mind. First, many people don’t seek medical attention for PPPs.
They are usually painless and not a health concern. So, they don’t get reported in medical databases.
Second, even if people notice them, they might not think to mention them to their doctor. They might assume they are normal or just ignore them. This means many cases remain undiagnosed or unreported.
Third, the definition itself can be slightly fluid. While doctors agree on the general appearance and behavior of PPPs, the exact size and number can vary widely. What one person calls a papule, another might see as a slight unevenness.
Studies that have been done are often on specific groups, like college students or clinic patients. These groups might not represent the general population perfectly. They can give us good estimates, but they aren’t definitive global counts.
The best we can do is rely on these studies and the general consensus among medical professionals. They indicate that PPPs are very common. It’s estimated that a significant percentage of adults will have them at some point in their lives.
Think of it as a common variation rather than a rare condition.
So, while we can’t give you a precise figure like “X million people have them,” we can confidently say they are widespread. The lack of exact numbers doesn’t make them any less real or any less common.
Challenges in Counting Piezogenic Pedal Papules
Asymptomatic Nature: Most people don’t report them.
Lack of Medical Seeking: Not seen as a medical problem.
Variability: Size and number differ greatly among individuals.
Study Limitations: Existing research is on specific demographics.
Broad Agreement: Professionals agree they are very common, even without exact data.
What the Future Holds for Understanding PPPs
As medical science moves forward, our understanding of common conditions like piezogenic pedal papules will continue to grow. While they might seem simple, further research can always reveal more insights.
One area of future exploration could be more detailed genetic studies. Pinpointing the specific genes and pathways involved could help us understand why some people are more prone to developing PPPs than others. This might even lead to better ways to predict risk.
Researchers might also look into the biomechanics of the foot more closely. How exactly does pressure distribute across the foot? Are there specific foot structures or gait patterns that are more strongly linked to PPPs?
Advanced imaging techniques could help here.
There’s also interest in the connective tissue itself. Understanding its precise composition and how it changes with age or certain activities could be valuable. This could inform how we approach skin and tissue health in general.
While treatments for PPPs are rarely needed now, if they were ever to become a significant issue for a larger group, or if linked to more serious conditions, research might explore therapeutic interventions. This could involve ways to strengthen connective tissue or manage fat distribution.
Ultimately, ongoing research aims to provide more clarity. Even for common, benign conditions, a deeper scientific understanding is beneficial. It helps us provide better information and reassurance to people.
It ensures that when something appears on our bodies, we have the knowledge to understand it.
For now, the consensus remains strong: PPPs are very common, generally harmless, and a normal variation for many feet. The continued study of them adds to our overall knowledge of skin and connective tissue health.
Future Research Directions for PPPs
Genetics: Identifying specific genes linked to PPPs.
Biomechanics: Studying foot pressure and gait patterns.
Connective Tissue: Analyzing its composition and aging process.
Therapeutics: Exploring potential treatments if issues arise.
Overall Knowledge: Enhancing understanding of skin and tissue health.
Conclusion
It’s completely understandable to feel curious or even a bit worried when you notice new bumps on your feet. Piezogenic pedal papules are one of those things that can cause a moment of alarm. But the good news is they are extremely common and usually cause no harm.
Knowing they are a normal part of how some feet respond to pressure can bring great peace of mind. If you ever have concerns, a quick chat with your doctor is always a wise step.